Helpful Products
Home Dialysis Central has pulled together this selection of helpful products for dialysis patients. Select a category to show only those related products. Do you have a product that you think could be useful for dialysis patients? Fill out this form to add it to our list.
Please note: we do not sell any of these products! You must contact the company that
makes them for price and order details. You will find contact info for each company under each
product.
Listings in the Helpful Products Catalog on Home Dialysis Central are a service to you. The Medical
Education Institute, its staff, its Board of Directors, and its sponsors do not endorse any product or
service. Talk with your doctor if you don't know whether a product is safe or wise for you to use. We do
strive to ensure that each listing is correct and complete—but, we can't guarantee it. We also can't
and don't endorse, recommend, or review all of the links you could follow off of this site to another site.
We are not responsible if a link you visit harms you or your computer, gives you wrong information, or if
any other loss or damange occurs.
Cath Dry



Cath Dry dressings significantly reduces the risk of catheter infections and allows the patient to SHOWER & even SWIM SAFELY between treatment sessions dramatically increasing the patients QUALITY OF LIFE. The dressing comes complete with an indication ring that turns RED if it comes in contact with water. The Cath Dry dressing is easy to apply however we would encourage you to visit our website for a video demonstration on how to best apply the dressing. Cath Dry is covered by Medicare and as a DME company on receipt of prescription we send the dressings directly to the patients home, we handle all the billing with zero cost to the patient . Shower again with confidence.
Submit an online prescription / order or download a pdf version here.
Contact Info
HEDclip



Contact Info
My Kidney Life: A New Direction


If your kidneys—or a loved ones’—don’t work well, you may be angry, sad, scared. Or, you may feel all three ways at the same time. This is 100% normal! When you can move past fear to HOPE, you can make the rest of your life as good as it can be. At the non-profit Medical Education Institute (MEl), we are here to help you. We’ve learned from tens of thousands of people with kidney disease and their loved ones. We use that knowledge to help YOU live as well as you can for as long as you can.
In this book, we teach you your job with a chronic disease. We help you sort out what matters to you. And, we tell you about each of the treatments, so you can make a choice that fits the way you want to live. We even have a free tool, My Kidney Life Plan, to help you match a treatment to your life. We hope you try it.
More Info and Purchase Options
Contact Info
How to Make a Killing-Blood, Death and Dollars in American Medicine



Six decades ago, visionary doctors achieved the impossible: the humble kidney, acknowledged since ancient times to be as essential to life as the heart, became the first human organ to be successfully replaced with a machine. Yet huge dialysis corporations, ambitious doctor-entrepreneurs and Beltway lobbyists soon turned this medical miracle into an early experiment in for-profit medicine—and one of the nation’s worst healthcare catastrophes.
Mueller evokes the scientific ingenuity and optimism of the 1950s and 1960s, when the burgeoning field of organ transplant and early dialysis machines offered long-awaited hope for lifesaving care. That is, until a New York salesman had himself dialyzed on the floor of the House, and Congress made renal disease the only “Medicare for All” condition—opening the financial floodgates for Big Dialysis. Of the thousands caught in a web of corporate greed, a disproportionate number are Black and Latino, highlighting the stark racial divides already endemic to American medicine.
How to Make a Killing reveals dialysis as a microcosm of American medicine and poses a vital challenge: find a way to fix dialysis, and we’ll have a fighting chance of fixing our country’s dysfunctional healthcare system as a whole, restoring patients, not profits, as its true purpose.
Contact Info
Silver Lining: Overcoming Adversity to Build NephroPlus

When kidney failure struck twenty-one-year-old Kamal Shah and threatened to derail his life, he fought back to take control. Dealing with each setback life threw at him with stoic bravery, Shah figured a way out each time. With lessons learnt dealing with the disease, he co-founded NephroPlus, a patient-centric dialysis company along with Vikram Vuppala, an MBA, and revolutionized dialysis care in India and beyond to become India’s largest dialysis services company. NephroPlus attracted marquee investors and created waves in the Indian healthcare ecosystem when they acquired US giant DaVita’s Indian operations. This book chronicles the entire journey right from Shah’s tryst with dialysis to the excitement of the investment rounds and the DaVita acquisition, and their road map for the future. It also provides useful insights into the healthcare ecosystem in India.
More Info and Purchase Options
Contact Info
MedAlerts Wristbands



The MedAlerts wristband with QR code technology provides access to your complete medical history to paramedics, nurses, doctors or law enforcement officers easily and securely.
Using a smartphone they can simply scan the QR code on the MedAlerts wristband to see all of the medical information you want them to know.
It eliminates the need for them to guess who you are, what medical conditions you have, what medications you are taking, etc. and increases your chance of getting the best care.
In an emergency situation wearing a MedAlerts wristband could save your life or the life of a loved one.
Contact Info
CarGenerator



CarGenerator is the World's First and Only Weatherproof Inverter.
CarGenerator is amazingly simple to use. 1. Start your engine, 2. Hookup CarGenerator 3. You have power for up to 80 hours
CarGenerator is the worlds lightest generator at 11 pounds.
Get a Discount on a CarGenerator for Your Home or RV—and Help MEI!
Readers can use these discount codes (the link will automatically apply them):
-
HOMEDIALYSIS150 - $150 off 1000w CG new
-
HOMEDIALYSIS250 - $250 off 1000w CG factory refurbished
-
HOMEDIALYSIS400 - $400 off Home Integration Kit bundle
The non-profit Medical Education Institute, which runs Home Dialysis Central, will receive a donation of $75 from CarGenerator if you purchase through this QR code or link: https://offer.cargenerator.com/homedialysis/.
Or just scan the QR code below!

Contact Info
Vidafuel® Wellness Protein

Contact Info
Pack-m-Ups™

Pack-m-Ups™ are a new kind of pill organizer and medication reminder. They are convenient and easy to use, and they work well as a daily, weekly, or monthly pill organizer.
Pack-m-Ups use a secure press-and-seal closure that makes it easy to open and close the moisture-resistant pill compartments. Pack-m-Ups are perforated so you can use them connected as a weekly pill organizer, or separate them to carry just what you need for the day.
Pack-m-Ups are made from a durable, flexible, and transparent material, so you can view your medications at a glance. And, you can personalize the write-on surface with a pen or marker to remind yourself of the day and time to take your pills. So, leave your pill box at home and use Pack-m-Ups when you are out and about, at work, shopping, or on extended business or pleasure travel.
Contact Info
RonWear Classic Ron Jacket



Comfortable active wear for patients with ports for dialysis, chemotherapy, transfusion and other infusion therapy.
Patent-pending dual-tab zipper applications in each arm make port connection easy, while staying dressed and warm! Zippers in each arm and on each side of chest for interchangeable port areas (or blood pressure check) when needed. Center zipper opening and back elastic waist for ease and comfort. Front pockets now with a media pocket to store and securely hold digital devices brought to treatment. 100% cotton brushed french terry is treated with a fluid repellant to make clean up easy! Available in either Dusk Blue or Charcoal Heather.
- The outfit is now ANTIMICROBIAL and won’t hold odors, WATER REPELLANT to resist blood or fluid stains, and has a STAIN RELEASE finish so it won’t hold stains in the garment
- Men’s sizes M–2X
- Women’s sizes S–2X
Contact Info
PD Solution Warmers

Properly-warmed solutions are simply healthier and more comfortable. All of Stickman’s warmers are calibrated at the factory to the optimal temperature for dialysis solutions—no adjustments are required by you. They are self-regulating, so you don’t have to worry about overheating them. All of our warmers plug into your vehicle’s cigarette lighter as well as any household outlet. 3 models to choose from. Made in Canada.
Take advantage of the freedom and independence that PD gives you—pack up your stuff and discover the wonders of the highways. And at home, our warmers work great, too (especially the Overnighter!): you won’t need to wait around the microwave or run back and forth to the kitchen. With a dedicated warmer next to your exchange area, a nice warm bag of solution is always within reach.
Contact Info
Immobilé

When it comes to securing PD transfer sets, simple is still best. Immobilé is one of the most innovative ways to secure PD transfer sets on the market. It remains the preferred choice for thousands of patients in the U.S., Canada, and Europe. A patented combination of hypoallergenic adhesive together with a Velcro hook-and-loop tab makes Immobilé cost effective, body trim, and very easy to use.
Immobilé was developed from patient requests for a device that not only secured the transfer set but that secured it in such a way as to allow normal active body movement (such as biking or skiing) without concern for the integrity of the set or access. Patients also wanted to eliminate the sticky step of pulling tape off the transfer set three or four times a day when releasing it for an exchange. When care is taken one Immobilé can be used for three days (up to 12 exchanges).
Many people prefer Immobilé to a belt because it is much more body trim, easier to use and yet, very effective.
Immobilé is:
- Easier and more cost effective than tape alone
- More body trim and less bulky than the belt
- Hypoallergenic
- Sterile product
- Available direct or through major distributors’ ancillary catalogs or formularies
Visit our website for more information and instructions for use. Email or call us to request a free sample.
Contact Info
Proteinex®



Proteinex® is a predigested liquid protein that provides a high content of protein (essential and non-essential amino acids) in a small serving size. 2 tablespoons (30 ml) will provide the patient with 15 grams of protein and 60 calories. Tablets provide the patient with 1 gram of protein per tablet. Proteinex® contains:
- NO sugar, NO fat, NO carbohydrates, and NO phosphorus
- No lactose or gluten
- Only 11mg of potassium and 4mg of sodium
- Ready to use; no mixing required
- Protein source: hydrolyzed protein collagen
- Predigested protein is easily absorbed (100%)
- May be used in patients with fluid restriction
- Promotes improved albumin levels
- Supplied in bottles of 8oz, 16oz, 30oz, and 120 Tablets
Proteinex®-18 is a predigested liquid protein that provides a high content of protein (essential and non-essential amino acids) in a small serving size. 2 tablespoons (30 ml) will provide the patient with 18 grams of protein and 72 calories. Proteinex®-18 contains:
- NO sugar, NO fat, NO carbohydrates, and NO phosphorus
- No lactose or gluten
- Only 13mg of potassium and 5mg of sodium
- Ready to use; no mixing required
- Protein source: hydrolyzed protein collagen
- Predigested protein is easily absorbed (100%)
- May be used in patients with fluid restriction
- Promotes improved albumin levels
- Supplied in bottles of 8oz, 16oz, and 30oz
Call Llorens Pharmaceutical at 866-595-5598 to obtain free samples.
Contact Info
Hemowear, LLC

Hemowear, LLC was created out of a desire to produce a clothing line that would help people with medical needs. This line of clothing will enable those who are on dialysis, and/or chemotherapy to feel confident and comfortable while receiving medical treatment. The clothing is customized for easy access to port sites, permanent catheter and AV fistulas.
Our mission is to design, manufacture and deliver products that meet the unique needs of each customer by marketing the most appealing and widely desired casual wear with the customers’ medical needs in mind.
Contact Info
RonWear Classic Ron Pant

Comfortable active wear for patients with ports for dialysis, chemotherapy, transfusion and other infusion therapy.
Femoral port openings in both legs with dual-tab zipper application that allows openings where you need them without undressing! Elastic waist pant with drawstring for extra comfort. Side and back pocket. Both men’s and women’s sizes come in Charcoal Heather or Dusk Blue with contrast stitching.
- Mens sizes M–2X
- Women’s sizes S–2X
- Now ANTIMICROBIAL and won’t hold odors, WATER REPELLANT to resist blood or fluid stains, and has a STAIN RELEASE finish so it won’t hold stains in the garment
Contact Info
Theraworx™

Theraworx is an all-natural solution designed to cleanse and nourish the skin. The skin-healthy formula lasts for hours after skin application, providing long-lasting moisture and protection. Containing no alcohols, it leaves your skin soft and comfortable rather than cracked and dry. Patented in 2002, this product has blossomed into a full line of skin-healthy products safe for the entire family, but strong enough for the clinician.
Theraworx is a skin-healthy solution to cleanse, moisturize, and protect your skin. The science behind the magic is multi-factorial and was designed over a period of years. First created by a dermatologist a decade ago, it has undergone a creation of its own. With ingredients included by category to perform numerous tasks, its base solution can be safely manipulated to become an entire line of products dedicated to meet the needs of the times.
Each ingredient is critical along with the methods used to provide a stable, reliable product. Theraworx is distributed only after undergoing a unique treatment process. This allows us to provide a product free of chemicals and alcohols so often used to prevent bacterial growth. Each ingredient is added in clinically significant amounts to assure function, not simply to look good on the label.
Contact Info
PD Belt
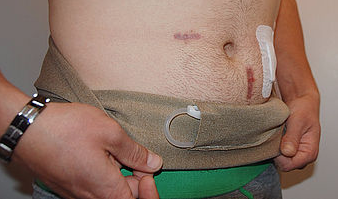


PD Belts - free shipping worldwide!
Our Peritoneal Dialysis Belt discreetly and securely holds the dialysis tube in place, giving you peace of mind.
Made with stretchy lycra, our PD Belt minimises the external appearance of your dialysis tube. The quick and easy velcro fastening makes it adjustable for maximum comfort and fit.
- Secure - safely holds the entire catheter tube in place
- Comfortable - no sagging or bulky seams
- Discreet - doesn’t show through clothes
- Durable - strong fabric that is machine washable
- Convenient - simple and easy to use
Available in beige and black, and in various sizes.
Contact Info
Dialysis Cart

The Dialysis Cart Model DC14 is specifically designed for PD patients. It provides easy access, helps organize, and helps with transporting your dialysis supplies. The DC14 is made of schedule-40 durable PVC and will never rust. It is also extremely durable, easy to clean, and is bacterial-static, meaning that bacteria will not grow or reproduce on the cart. Warranty: 5 years on frame, 2 years on casters and fabric. Ships via UPS.
Model DC14 features:
- 43" H x 34" W x 16" D
- Specially designed for PD patients
- Sturdy 4-drawer cart with 2 shelves
- Easy-roll 3" dual-wheel casters (2 locking)
- Available in redwood (shown in picture)
Click here to see this product on the manufacturer’s website.
Contact Info
Champion Chair Dialysis Recliner

Champion Manufacturing is a leading supplier of patient seating to all of the nation’s largest dialysis providers. The features that have made our recliner a best-seller in dialysis centers are the same features that make it well-suited for the home dialysis patient: comfort, quality, durability, and ease of operation for patients and their caregivers. Infection control is critical to the home dialysis patient, and Champion’s dialysis recliner with antimicrobial vinyl upholstery and quick-release seats make cleaning and disinfecting surfaces easy. Champion ships via white-glove carrier to patient homes in most areas. Recliners are fully assembled and ready to use when they arrive.
Contact Info
Alcavis Bleach Wipes

Portable | Accessible | Convenient
- COVID-19 Protective as per the CDC Requirements for Disinfectants
- Ideal for blood and body fluid spills
- Eradicates C. difficile, S. aureus, S. enterica, P. aeruginosa, TB & HIV: Viral, MRSA and VRE, Norovirus
- Fast-acting kill power against resistant pathogens
- Stable: 12-month shelf life
- Consistent and accurate concentration of bleach every time
- CDC & OSHA compliant
Contact Info
RonWear Classic Jacket & Pant Set



Comfortable active wear for patients with ports for dialysis, chemotherapy, transfusion and other infusion therapy.
- 4-port jacket with zippered pant for femoral ports OR no-zipper pant
- Jacket has a Media Pocket inside the front pocket to securely hold digital devices brought to treatment
- The outfit is now ANTIMICROBIAL and won’t hold odors, WATER REPELLANT to resist blood or fluid stains, and has a STAIN RELEASE finish so it won’t hold stains in the garment
- Women’s sizes: S–2X
- Men’s sizes: M–2X
Both men and women’s sizes come in Dusk Blue or Charcoal Heather with contrast stitching.
Contact Info
MyMedSchedule™

MyMedSchedule™ is a great medication reminder and is free! Your personal medication chart clearly shows the times you should take each medicine or supplement, and how much to take. There are even images of your pills so there is no confusion.
You can place a medication chart where you will most need it: either on the refrigerator, or in your bedroom or bathroom. And if you travel, or are just out for the day at work or shopping, you can take the wallet-size MyMedSchedule list with you.
With MyMedSchedule, you even have an easy way to share your medication list with all of your doctors and dentist, and the schedule is readily available in case of an emergency. One MyMedSchedule.com user tells us, "My doctors love it when I bring my chart to each visit so they can quickly see everything I am taking."
Try this free program by going to www.mymedschedule.com. You can start with your current meds, and easily update your medications as often as you need. You can even create a schedule for your other family members.
You can rest easy as your medical information remains secure with MyMedSchedule. Your personal health information is protected by SSL encryption, and will not be redistributed or resold.
Contact Info
Enviro-Pad

The Enviro-pad is an economical, multi-purpose, highly absorbent, disposable fluid barrier pad with a laminated backing that absorbs an amazing 1,000 ml per square yard. The air-spun material provides enhanced comfort and has a multitude of practical purposes in and out of the medical field.
Key benefits include:
- Fluid capacity of 1,000 ml per square yard
- Fluid absorption rate of 6.1 seconds/10 ml
- Laminated backing that prevents fluid strike-through
- Reversible for emergency spills
- Adhesive at corners for securing purposes
- Assists with waste disposal by incinerating to a fine ash
- Facilitates faster O.R. clean-up and turn-around
- Enhanced comfort while standing assists in reducing leg stress
- Economically priced
- Versatile and practical
- Performs well for chemical spill protection
- Equipment and floor protection from liquid contaminants
- Lengths may be customized to preference
Contact Info
5 Simple Steps to doing PD Successfully

This powerful, uplifting pocket book is a simple and effective tool that is an easy read. It confronts so many of the problem areas faced by PD patients, including:
- Catheter Placement
- Organizing Monthly Supplies
- How to keep Your Pets While Doing Peritoneal Dialysis
- Myth Busters and Tips to Review with Your Medical Team
The tips will not only help you with coping with peritoneal dialysis, but also will enlighten your medical team, friends, nurses, family members, and caregivers in their efforts to make life more comfortable for you.
If you or your loved one is considering doing peritoneal dialysis or recently started peritoneal dialysis, this book is a must-read!
About the Author
Sheila Shaw has been living with chronic illnesses for the past 20 years. As the CEO of Patient’s Pride, Inc., a kidney transplant recipient, and a former peritoneal dialysis patient, and after speaking with thousands of PD patients and successfully helping them support their catheters and move forward with their lives, Sheila Shaw knows from personal and professional experience how to truly get through peritoneal dialysis successfully. Sheila has dedicated her life to inspire others to live their lives to their fullest despite living with chronic illness.
Contact Info
Redsense Blood Detector

The Redsense safety device is designed to detect venous needle dislodgement during hemodialysis, for Home/Self and Clinical use.
Redsense consists of two parts: a sensor patch and an alarm unit. An infrared signal is transmitted from the alarm unit to the sensor patch using fibre optic cable. In the event of bleeding, inner layers of the patch smear blood over the optical sensor, which triggers the alarm.
The Redsense safety device is the results of close co-operation between medical staff and engineers. Dialysis equipment today is required to have a system which protects the patient from blood loss due to dislodgement of the venous needle. The commonly accepted solution is to monitor by the venous pressure alarm but a better solution has long been requested. Even with the routine supervision of medical staff still the venous needle can become dislodged: the dialysis machine will then continue to draw blood from the patient’s artery however not returning blood in the loop circuit as the venous needle has become dislodged and the patient’s blood ends up elsewhere. If undetected, this blood loss can have very serious consequences in only a few minutes. Redsense safety device provides a solution to this problem and detects venous needle dislodgement instantaneously; it only takes a few milliliters of blood on the sensor patch to sound the alarm.
Optimizing safety conditions for home hemodialysis users is a core ambition for Redsense Medical.
Redsense Medical has offices in Sweden and in the U.S. (Chicago, IL). For more information: www.redsensemedical.com.
Contact Info
Cool Blue Wave Premium Tuck-away Belt

Contact Info
JMS AV Fistula Needles

JMS develops dialysis products promoting the safety and welfare of healthcare workers and patients. JMS provides several brands of AV fistula needles to meet any clinical need. They are proud to offer the following products for dialysis:
SysLoc® Family
The
simple and effective design of the SysLoc family allows the needle to retract easily into the hub without the use of any bulky attachments. The SysLoc needle allows you to choose from a wide range of configurations for hemodialysis or apheresis treatments.
WingEater®
The
JMS WingEater is our most popular safety AV fistula needle. WingEater provides extraordinary needle-stick protection in an easy-to-use design.
Harmony™
The
JMS Harmony needle is for use with previously-established mature access sites using a constant-site (Buttonhole) technique of needle insertion. JMS Harmony needles include an innovative site preparation tool and is specifically designed for home dialysis patients and patients who self-cannulate.
Please contact JMS or one of their distributors for more information. You can also visit their website for video and training manuals.
Contact Info
Chef Paul Prudhomme's Magic Seasoning Blends

Chef Paul Prudhomme’s Magic Seasoning Blends® has been in business since 1983 and has grown to fill a 125,000-square-foot plant, blending and shipping Chef Paul’s dry spices, rubs, bottled sauces, and marinades.
For those who are looking for dialysis-safe, all-natural, no-salt, no-sugar seasoning blends, look no further! They are also no-MSG and gluten-free. Available flavors include Lemon & Cracked Pepper, Sweet & Spicy, Seven Herb, Toasted Onion & Garlic, and Six Spice.
Contact Info
PD Panty/PD Brief
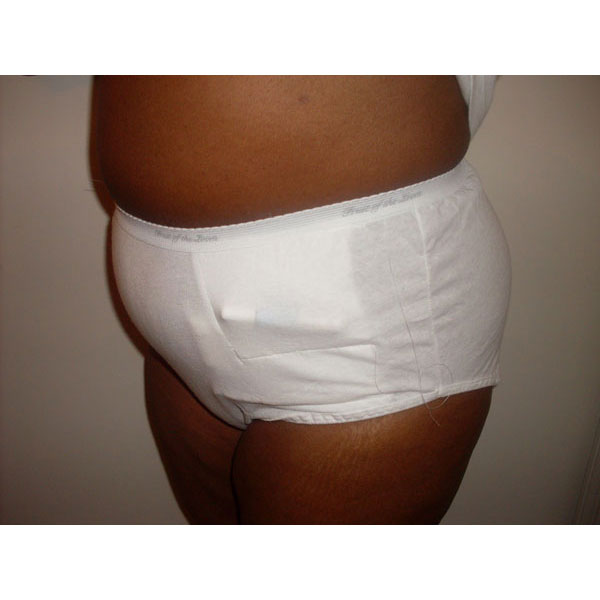

The PD Panty comes in two styles: day and night.
The "day" version has of a pocket for the port at the end of the transfer set tubing to rest in that is just below the waist band on the inside of the garment. A "guide" that is open at both ends serves as a guide for the transfer set tubing to "thread" through and rest in the pocket above the guide in the inside of the panty. This protects the exit site from being injured by pulling of the tubing, as well as keeps the transfer set tubing from dangling.
When wearing the PD Panty, the port and transfer set tubing is not visible from the outside of the under garment. The panty provides safety, comfort, convenience, and a sanitary means of caring for the exit site. Made of cotton and cotton blends, the panty can be washed and cleaned with regular laundry detergent. Available in sizes from small to XX large.
The "night" version consists of the pocket on the outside and guide on the inside. The additional feature of the PD Panty "night" is that the garment has a button hole on the side of the garment between the guide and the pocket to allow the transfer set tubing to thread through the guide and come out to the outside of the garment through the button hole. The port again rests in the pocket on the outside of the garment. The garment is called the PD Panty "night" because the button hole allows the patient to connect to the Cycler without having to pull the underwear off or pull the underwear down. The guide protects the connection as the patient dialyzes and or sleeps. The PD Panty "night" can be worn at any time.
Contact Info
CELOX Hemostatic Products



FDA-Approved CELOX [CELL-ox] Products are redefining effective bleeding management. Bleeding has been stopped in much the same way it has been since the turn of the last century – until now. CELOX Granules, Gauze and Dressing are invaluable, potentially life-saving products that provide rapid, efficient hemostasis for men, women, children and seniors.
CELOX provides a range of hemostatic products to control bleeding from and around central venous catheter, fistula, and graft access sites. CELOX performance has been proven on the battlefield, in emergency and clinical settings, and in the laboratory.
CELOX is the only hemostat proven to rapidly stop bleeding even when blood and its ability to clot is compromised by use of anti-coagulant blood thinners like Coumadin, Warfarin, Plavix, Pradaxa or Xarelto. CELOX doesn't sting or burn and easily irrigates with water or saline.
CELOX products are not new. CELOX was created for use on military battlefields to stop severe bleeding in its tracks – in most cases instantaneously – even in extreme circumstances or challenging conditions. Now the same FDA-approved, military-strength, hospital-grade products are available for use in non-military markets – without a prescription. CELOX is classified by the FDA as an OTC medical device, not a pharmaceutical.
- In the history of its use, there have been no reports of CELOX having failed or underperformed
- CELOX – FDA /Health Canada/NATO approved & prestigious Class 3CE mark in Europe
- Classified by FDA as an OTC medical device, not a pharmaceutical – for nosebleeds and minor, moderate and severe bleeding [not yet available in retail stores]
- Only product proven to quickly stop bleeding for those on blood thinners like Coumadin, Warfarin, Heparin, Plavix, Pradaxa or Xarelto
- Each product designed to be easily self-administered and used by those with no emergency or medical training
- Cannot be over-used – No measuring or "dosing" needed
- Reduces risk related to spread of blood-borne pathogens
- Works for those with inherited or acquired bleeding or clotting disorders [like Hemophilia]
- Does not sting, burn or generate heat
- Easily washes away with water or saline – no debridement necessary
- Because it is bio-compatible, remaining CELOX granules are safely absorbed
Free shipping when you enter code HDCfreeshipping at checkout.

