When To Start Dialysis
When you know your kidneys are failing, it's normal to want to put off dialysis forever. Common wisdom used to say that starting dialysis early was best for you. The funny thing about common wisdom, though, is it could turn out to be wrong. Research now suggests that putting off dialysis as long as you can may be the safer choice.
Stages of chronic kidney disease
The National Kidney Foundation's (NKF) guidelines 1 have divided chronic kidney disease (CKD) into five stages based on glomerular filtration rate (GFR), roughly the measure of your percent kidney function:
| Stage of CKD | GFR (mL/min) | Action to take |
|---|---|---|
| 1 | ≥ 90 |
|
| 2 | 60–89 |
Estimate the rate at which your CKD is progressing |
| 3 | 30–59 |
Evaluate and treat any complications |
| 4 | 15–29 |
Prepare for transplant or dialysis |
| 5 | < 15 |
Start dialysis or get a transplant (if uremia is present) New evidence says dialysis should start by a GFR of 6, or sooner if there are symptoms. |
Uremia is a build-up of wastes in the blood. As kidneys fail, this build-up of wastes and excess water in the blood causes symptoms, like:
- Overwhelming fatigue
- Itchy skin (the itching may be so severe that it can wake you up at night)
- Swelling in your hands, feet, or face
- Loss of appetite, nausea, vomiting, eating less (or no) protein, "metal" taste in your mouth
- Feeling faint or dizzy
- Trouble with mental focus
- Feeling cold when others are warm
- Shortness of breath
The symptoms people have as their kidney function gets worse can vary a lot. Some people even feel fine and report no symptoms. For many years, the choice of when to start dialysis was as much an art as it was a science. Doctors would decide with their patients when blood test values and symptoms warranted starting treatment.
When the NKF guidelines came out in 1996, doctors began to say that CKD 5 was kidney failure. When the GFR dropped to 15 mL/min, dialysis should start. 2 They were wrong.
New research to guide your choice

In 2004, researchers began the Initiating Dialysis Early and Late (IDEAL) study. 4 The plan was to recruit 800 people with CKD and follow them for three years to find out who would live longer:
- Those who started dialysis early, at a GFR of 10–14 mL/min, or
- Those who started dialysis late, at a GFR of 5–7 mL/min.
The findings of the IDEAL study are now out, 5 and they are not what most nephrologists expected. Of the 828 people who were randomly chosen to start treatment early or late:
- 404 people started early, and 152 (37.6%) died.
- 424 people started later, and 155 (36.6%) died.
There was no significant difference in survival between the two groups. And, the late-start group got to have an extra six months or so off of dialysis!
Three other non-random studies have found that starting dialysis early does not help you—and it may even be harmful.
- A French study of 541 people done in 2005–2006 found that late starters had more illnesses and a higher risk of emergency dialysis starts. However, they lived just as long as early starters. 6
- A Swedish study followed 901 people who chose to start dialysis early or late. Late starters were 84% more likely to survive than those who started early. 7
- A U.S. study found that starting dialysis earlier may be harmful for patients. Researchers looked at survival of 81,176 people who did not have diabetes. The risk of death went up the earlier dialysis began. Those who started treatment with a GFR of 5.0–9.9 mL/min were more than twice as likely to live. 8
Based on these studies, a new position statement from the UK 9 says dialysis needs to start with a GFR of 6. It can start sooner if there are symptoms of uremia. People at high risk (with diabetes or heart disease) may also want to start sooner. And, there are steps you can take to boost your chances of feeling well as long as possible.

1. See a nephrologist
A number of studies have found that people with CKD who see a nephrologist (kidney specialist) do better. A nephrologist can: 10
- Help you learn about your health problem
- Offer treatments to prevent or help slow the rate of kidney failure
- Teach you about treatment options
- Help ensure that you get a dialysis access placed in time for your treatment choice
Seeing a nephrologist early can help give you the best chance of slowing your CKD. A 1999 study looked at 135 people whose kidneys failed. 11 The 105 who saw a nephrologist at least four months prior to starting dialysis:
- Had better nutrition,
- Got more treatment for anemia (a shortage of red blood cells that can leave you feeling tired and cold all the time),
- Were more likely to have an access.
A larger study of 2,264 people looked at those who saw a nephrologist at least twice in the year before dialysis vs. those who didn't. Those who did see one were much likelier to be alive two years later. 12
2. Know your blood tests

Sometimes people don't want to make a fuss and ask the doctor's office for their blood test results. But those results belong to you—and you need them to know how you're doing.
If you know your serum creatinine (a waste removed by healthy kidneys) level, for example, you can learn your GFR. A number of online calculators will help you figure it out. Type " GFR calculator" into Google and take your pick.
Some people keep a notebook, either on paper or on a computer, to track their lab test results. This is a good way to keep track of your medications, too.
3. Know your symptoms

You are an expert in you—how you feel from day to day, what makes you feel better or worse, etc. Learn the symptoms of CKD and observe yourself to see if you have any of them. If you do, make a note of them for your doctor. Be sure to include things like:
- When did the symptom first start?
- Do you have it all the time, or just some of the time (if so, when)?
- Does anything make the symptom better or worse?
4. Eat some protein—and other good foods

When your kidneys are failing, you may not want to eat protein (meat, eggs, chicken, etc.). This can be a symptom of uremia. You need to get some protein, however. In a large U.S. study, people with CKD who ate a very low-protein diet did not live as long as those who ate more. 13
People often want to know what they can eat to fix their kidneys. There are no magic foods that will do this—so use common sense. Fresh foods, like vegetables and fruits, are better for you than processed or fried foods. The fewer ingredients a food has, the closer it is to being real food.
In a small study, a diet free of gluten (found in wheat) was found to protect the kidneys of children who had diabetes and Celiac disease. 14 A number of other small studies have also suggested that there may be a link between gluten and kidney disease.
5. Get a dialysis access placed
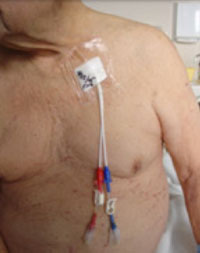
You may not need to start dialysis or get a transplant until you have a GFR of 6 and if you don't have symptoms. But if you'll need dialysis, you need a way to get access to your blood so it can be cleaned. You do not want to start treatment with a central venous catheter (CVC) if you can help it.
A CVC is a plastic tube that is placed in a central vein in your chest, with the tip inside your heart. Two "ports" dangle outside of your skin. Because it is both outside and inside your body, a CVC is an open door for germs. The risk of sepsis (blood poisoning), which can be fatal, is far higher with a CVC than with other, better types of access for hemodialysis. The NKF guidelines suggest getting an access at stage 4 CKD. This allows time for it to heal and be ready to use when the day to start treatment comes.
Better choices for dialysis access are:
Conclusion
Talk with your doctor about your health—and when to start dialysis or get a transplant, based on your blood tests and symptoms. It may be later than you think.References:
- KDOQI Clinical Practice Guidelines for Chronic Kidney Disease: Evaluation, Classification, and Stratification Part 4, Guideline 2; Accessed Aug. 25, 2011.
- Ortega LM, Nayer A. Repercussions of early versus late initiation of dialysis. [Article in English, Spanish] Nefrologia. 2011 Jul 7;31(4):392–396.
- Churchill DN. An evidence-based approach to earlier initiation of dialysis. Am J Kidney Dis. 1997 Dec;30(6):899–906.
- Cooper BA, Branley P, Bulfone L, Collins JF, Craig JC, Dempster J, Fraenkel MB, Harris A, Harris DC, Johnson DW, Kesselhut J, Luxton G, Pilmore A, Pollock CA, Tiller DJ; IDEAL Study Steering Committee. The Initiating Dialysis Early and Late (IDEAL) study: study rationale and design. Perit Dial Int. 2004 Mar–Apr;24(2):176–81.
- Cooper BA, Branley P, Bulfone L, Collins JF, Craig JC, Fraenkel MB, Harris A, Johnson DW, Kesselhut J, Li JJ, Luxton G, Pilmore A, Tiller DJ, Harris DC, Pollock CA, for the IDEAL study. A randomized, controlled trial of early versus late initiation of dialysis. N Engl J Med. 2010 Aug 12;363(7):609–19.
- Thilly N, Boini S, Soudant M, Kessler M, Briancon S, Frimat L. Outcomes of patients with delayed dialysis initiation: Results from the AVENIR study. Am J Nephrol. 2011;33(1):76–83.
- Evans M, Tettamanti G, Nyren O, Bellocco R, Fored CM, Elinder CG. No survival benefit from early-start dialysis in a population-based, inception cohort study of Swedish patients with chronic kidney disease. J Intern Med. 2011 Mar;269(3):289–98.
- Rosansky SJ, Eggers P, Jackson K, Glassock R, Clark WF. Early start of hemodialysis may be harmful. Arch Intern Med. 2011 Mar 14;171(5):396–403.
- Tattersall J, Dekker F, Heimburger O, Jager KJ, Lamiere N, Lindley E, van Biesen W, Vanholder R, Zoccali C, on behalf of the ERBP Advisory board. When to start dialysis: updated guidance following publication of the Initiating Dialysis Early nad Late (IDEAL) study. Nephrol Dial Transplant. 2011;26:2082–86.
- Obrador GT, Pereira BJ. Early referral to the nephrologist and timely initiation of renal replacement therapy: a paradigm shift in the management of patients with chronic renal failure. Am J Kidney Dis. 1998 Mar;31(3):398–417.
- Arora P, Obrador GT, Ruthazer R, Kausz AT, Meyer KB, Jenuleson CS, Pereira BJG. Prevalence, predictors, and consequences of late referral at a tertiary care center. J Am Soc Nephrol. 1999;10:1281–6.
- Stack AG. Impact of timing of nephrology referral and pre-ESRD care on mortality risk among new ESRD patients in the United States. Am J Kidney Dis. 2003 Feb;41(2):310–18.
- Menon V, Kopple JD, Wang X, Beck GJ, Collins AJ, Kusek JW, Greene T, Levey AS, Sarnak MJ. Effect of a very low protein diet on outcomes: long-term follow-up of the Modification of Diet in Renal Disease (MDRD) Study. Am J Kidney Dis. 2009 Feb;53(2):208–17.
- Malalasekera V, Cameron F, Grixti E, Thomas MC. Potential reno-protective effects of a gluten-free diet in type 1 diabetes. Diabetologia. 2009 May;52(5):798–800.

