PD - Separating Myth from Fact
Is it possible to do peritoneal dialysis (PD) if you can only use one arm? If you're blind? You can't hear? What if you have a hernia? If you're 87 years old? A transplant failed? The answer to all of these (and more!) is YES.
According to published research, many people who might not be given the option of PD can, in fact, succeed with it. So, let's look at PD and clear up some common myths.
I can use only one arm
To do PD, you need to be able to connect your PD catheter to the PD bags. There's no doubt that this is easier with two hands. But you don't need two. With an assist device to hold the tubing in place, you can safely connect with one hand.
 )
More than 10 years ago, a dialysis center in Indiana found a way to help a patient use the Baxter Ultrabag system with one hand. Baxter engineers then used it to create the EZ-Aide Assist Device®.
1
Your PD nurse can order this today—it's Baxter item number 5C4505.
2
)
More than 10 years ago, a dialysis center in Indiana found a way to help a patient use the Baxter Ultrabag system with one hand. Baxter engineers then used it to create the EZ-Aide Assist Device®.
1
Your PD nurse can order this today—it's Baxter item number 5C4505.
2
Your center uses Fresenius PD supplies? No problem. The Stay.Safe® system has one connection. A control dial guides you through the treatment steps. A patient who had only the use of his left arm was able to do PD by himself using the Stay.Safe. 3 This two-bag system is easy to learn and use.
I'm blind
You are not alone if you want to do PD and you can't see. More than 40% of the people on dialysis in the U.S. have diabetes, which can cause vision loss along with kidney damage.
At this time, Most PD cycler screens don't talk. We hope talking screens will be a feature that all PD companies will add soon. Currently, the Amia cycler does have the ability to talk to patients. Blind people also have been able to use CAPD, where exchanges are done by hand. In fact, in a British study, blind patients had less peritonitis (infection) and fewer PD problems than sighted patients. 5
In one case study, a blind woman wanted to do PD so she could care for her young daughter. With a talking scale and blood pressure cuff, and the Fresenius Premier™Plus double-bag system, she learned to do PD. EPO was given in prefilled syringes so she did not have to have someone draw up the dose she needed. She was taught to call her PD nurse if she had any abdominal pain that might mean peritonitis. 6 This same system has been used with success in Canada to train blind people to do PD.
In Poland, a program was started to train blind people to do CAPD, also using a two bag system. They had good results, with just one case of peritonitis per 28 months of PD. 8 A 10-year study found that keys to survival and PD success in blind and other patients were:
- Patient motivation
- Acceptance of health problems
- Staff willing to train patients
In this study as well, blind patients did as well as sighted ones. 9
You may have to search for a center that will train you for PD. Your nurse will need to feel that you can learn the steps and do them in order without risking infection. Using a tape recorder to take notes during training can help you recall the steps.
I'm hearing impaired
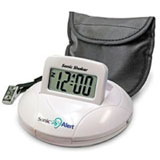 It's no problem to do CAPD if you can't hear. But can you use a cycler? With a bit of creativity, the answer can be yes. A center in Philadelphia changed the standard alarm on a PD cycler from a beep to a vibration. They used a Sonic Alert Wake Up Alarm with a Sonic Alert Super Shaker Bed Vibrator.
10
With a vibrator pad under the pillow or mattress, you can feel the alarm and wake up to take action.
It's no problem to do CAPD if you can't hear. But can you use a cycler? With a bit of creativity, the answer can be yes. A center in Philadelphia changed the standard alarm on a PD cycler from a beep to a vibration. They used a Sonic Alert Wake Up Alarm with a Sonic Alert Super Shaker Bed Vibrator.
10
With a vibrator pad under the pillow or mattress, you can feel the alarm and wake up to take action.
I have a hernia
A hernia is a weak spot in the muscle of your belly. On PD, a hernia can be a problem if pressure from fluid in your abdomen traps part of your peritoneum in the weak spot—or if PD fluid leaks into your groin. Can you do PD with a hernia? Yes, but you will need to have it fixed.
Among 122 patients who started CAPD from 1994 to 2001, 17.2% had a hernia (some even had more than one). Nearly three-fourths were found before PD was started. 11 (In a Polish study, 10% had hernias.12) Most were fixed under local anesthesia with mesh to repair the weak spot, and a PD catheter put in at the same time. Another study of 46 patients who had hernias fixed found that only one had to change to hemodialysis (HD). This study found that the mesh repair was safe and effective. 13
If you get a hernia after you start PD, you don't have to change to HD while it is fixed. A recent study looked at hernia repairs on PD over 10 years. Patients had no dialysis for 48 hours after surgery. Then, CAPD patients did PD three days per week for two weeks, and five low volume (1-1.5 liter) exchanges per day for two more weeks. Then they went back to their normal schedule. Cycler patients did PD three days per week for a week, then three nights per week for four weeks, then went back to normal. No patients had a leak or an early recurrence of a hernia. 14
Lying flat to do PD exchanges while you heal from a hernia repair can reduce the pressure on your stitches. It takes 6 weeks for new collagen to fully form so the repair is stable, so lying down for PD during this time may help reduce the chance of your hernia coming back. And, of course, after a hernia is fixed, you will need to strictly follow any limits you are given on lifting, jumping, driving, straining to have a bowel movement, or any other task that would raise the pressure in your belly.
I'm 87 (or 93)
 Age alone should not keep you from doing PD. PD can allow you to stay more independent, and may help you keep your remaining kidney function longer.
15
A review of medical studies found that most older patients had the hand-eye and thinking skills needed to do PD. Plus, they tended to follow their treatment plans very closely.
16
Older PD patients did not have any more PD problems than younger ones.
17
Age alone should not keep you from doing PD. PD can allow you to stay more independent, and may help you keep your remaining kidney function longer.
15
A review of medical studies found that most older patients had the hand-eye and thinking skills needed to do PD. Plus, they tended to follow their treatment plans very closely.
16
Older PD patients did not have any more PD problems than younger ones.
17
Studies of PD patients in their 80s 18 and 90s 19 found few PD-related problems—and just one hospital stay per 2.5 patient years (not only for dialysis). While most did need some help at home, the authors say PD is safe and suitable in old, old patients. 18
If you live alone, you would need to be able to lift the bags onto the cycler or an IV pole for CAPD. Joint pain in your hands or nerve damage so that you can't feel your fingers would also make it hard to do PD without help.
I have no kidney function
If you have had your kidneys removed or been on dialysis long enough not to have any kidney function, studies show that you can still safely do PD.
Guidelines for dialysis say how much treatment you should get. 20 For CAPD, you need:
- A Kt/V urea of at least 2.0
- A creatinine clearance of at least 50-60 liters/week/1.73 m 2
For CCPD (with a cycler), you need:
- A Kt/V urea of at least 2.1
- A creatinine clearance of at least 63 liters/week/1.73 m 2
If you are a large, tall, muscular—but not overweight—person with no kidney function, you may not do well on PD. If you do choose PD, keep a close eye on your appetite for protein: losing your taste for meat is a sign that you may not be getting enough treatment. Other signs may include:
- Trouble sleeping
- Bad taste in your mouth
- Itching
- Depression
- Swelling
- Fatigue
You might also think about doing home HD instead of PD.
When you don't have kidney function, your doctor needs to know how well your peritoneum is working as a filter. Over time, it can stop working as well. You can tell that this is happening if you can't drain out as much fluid as you put in. Long term use of PD fluid based on sugar can harm the membrane—and higher glucose bags make this happen faster. Use of icodextrin PD fluid can slow the damage to the peritoneal membrane so you may be able to do PD longer. 21
With no kidney function, if the day comes when you can't do PD any more, you may want to think about daily or nocturnal HD—options that give you more treatment, more independence, and fewer limits on diet and fluids than standard in-center HD.
My transplant failed
When you're used to being independent with a transplant, going to a center three times a week for HD can take away your sense of control. PD can put you back in the driver's seat of your own life.

One study compared 34 PD patients with a failed transplant to 82 PD patients who never had a transplant. The groups had similar age, sex, remaining kidney function, and PD dose. None had diabetes. Survival at 1 year, 3 years, and 5 years was slightly higher in the failed transplant group. Somewhat fewer of the failed transplant patients were able to keep doing PD. 22
Another study compared all patients who started PD after a failed transplant from 1989 to 2001 to:
- New PD patients
- Failed transplant patients who chose HD
There were no survival differences between the groups, and no difference in the number who were able to keep doing PD. 23 An Australian study of PD after transplant failure vs. new PD patients found the same things. 24 So did a study from Belgium. 25
I am overweight
These days, a lot of Americans are overweight, and that includes people with kidney failure. In fact, since so much kidney failure is caused by type 2 diabetes, many people on dialysis are overweight. So, can you do PD?
Well, yes, but you have to be careful. PD catheter infections are more likely. Using a presternal PD catheter—placed in the chest instead of the belly—can help reduce this risk. 26 Overweight people also have a much higher risk for peritonitis, though the reasons why are not clear. 27 A 2-year study of heavy vs. normal people on PD found no survival differences. 28 But, an Australian study looked at 9,679 PD patients at four levels of weight:
- Obese (body mass index (BMI) ≥30)
- Overweight (BMI of 25 to 29.9)
- Normal (BMI of 20 to 24.9)
- Underweight (BMI <20)
The authors found lower survival rates in obese PD patients and suggested close follow-up to be sure all is well. 29 This study did not look at HD, so we can't say whether obese patients would have done better on that treatment. The larger you are, the more treatment you need, so standard in-center HD is not likely to be enough.
If you are overweight and have diabetes, PD seems to be a better choice if you are younger—not older. A review of large studies found that in the U.S., if you are older than 45 and have diabetes, you are likely to live longer on HD than PD. In other parts of the world, survival was the same for both treatments. 30
I've had peritonitis
Can you still do PD after a bout of peritonitis? Maybe. Sometimes the infection can scar your membrane so PD is impossible. This is a reason to catch it as early as you can by watching for cloudy bags, abdominal pain, or fever. A recent study looked at people who had peritonitis in their first three months of PD vs. a group that didn't. The early peritonitis group was almost twice as likely to die or to have to change to HD as the others. 31 This suggests that good training and technique are vital.
Another new study divided 106 PD patients who'd had peritonitis into four groups:
- Group 1 (42 people) had their PD catheter put back in
- Group 2 (16 people) chose to switch to HD
- Group 3 (35 people) had to switch to HD
- Group 4 (13 people) died within four weeks
In Group 1, 23 of the 42 people were able to safely restart PD. 32 So, it is sometimes—but not always—possible to do PD after peritonitis.
Conclusion
Since you are the one who will have to live with your treatment choice each day, you need to be able to choose a treatment that will fit your life. If PD is what you want, don't let yourself be screened out by rules that may be based on prejudice rather than science. When someone says you can't do PD, be sure there is a valid reason why not.
You may have to look around to find a center that will support you, but nearly one out of three of the 4,700 dialysis centers in the U.S. offers PD. With a little effort, you can find one that may be able to help you succeed on PD.
References:
- Berger M. Performing CAPD independently with one hand using an assist device. ANNA J. 1996 Dec;23(6):618-22.
- Baxter online catalog. Accessed May 22, 2007.
- Schuetz CE. Training a continuous ambulatory peritoneal dialysis patient with one functional arm. Adv Perit Dial. 2005;21:146-7.
- Lambert MC, Lage C, Kirchgessner J. Stay.safe. A new PVC free system in long-term CAPD treatment. EDTNA ERCA J. 1999 Jul-Sep;25(3):30-4.
- Flynn CT. Why blind diabetics with renal failure should be offered treatment. Br Med J (Clin Res Ed). 1983 Oct 22;287(6400):1177-8.
- Wright LS. Training a patient with visual impairment on continuous ambulatory peritoneal dialysis. Nephrol Nurs J. 2005 Nov-Dec;32(6):675,666.
- Bentley ML. Keep it simple! A touch technique peritoneal dialysis procedure for the blind and visually impaired. CANNT J. 2001 Apr-Jun;11(2):32-4. Comment in: CANNT J. 2001 Oct-Dec;11(4):8.
- Pietrzak B, Olszowska A, Wankowicz Z. [Continuous ambulatory peritoneal dialysis as a renal replacement therapy in blind diabetics with type 1 diabetes] [Article in Polish] Pol Merkur Lek.arski 1998 Nov;5(29):271-3.
- Chandran PK, Lane T, Flynn CT. Patient and technique survival for blind and sighted diabetics on continuous ambulatory peritoneal dialysis: a ten-year analysis. Int J Artif Organs. 1991 May;14(5):262-8.
- Kushner A. Adaptation of the Fresenius PD+ Cycler for a hearing-impaired patient. Adv Perit Dial. 2000;16:163-4.
- Garcia-Urena MA, Rodriguez CR, Vega Ruiz V, Carnero Hernandez FJ, Fernandez-Ruiz E, Vazquez Gallego JM, Velasco Garcia M. Prevalence and management of hernias in peritoneal dialysis patients. Perit Dial Int. 2006 Mar-Apr;26(2):198-202. Comment in: Perit Dial Int. 2006 Mar-Apr;26(2):178-82.
- Smietanski M, Renke M, Bigda J, Smietanska I, Rutkowski B, Witkowski P, Sledzinski Z. Management of inguinal hernia on peritoneal dialysis: an audit of current Polish practice and call for a standard. Int J Artif Organs. 2006 Jun;29(6):573-7.
- Johns EM, Poole G. Gs20p single-centre experience with mesh repair of abdominal hernia in CAPD patients. ANZ J Surg. 2007 May;77 Suppl 1:A30.
- Shah H, Chu M, Bargman JM. Perioperative management of peritoneal dialysis patients undergoing hernia surgery without the use of interim hemodialysis. Perit Dial Int. 2006 Nov-Dec;26(6):684-7.
- Winchester JF. Peritoneal dialysis in older individuals. Geriatr Nephrol Urol. 1999;9(3):147-52.
- Teitelbaum I. Peritoneal dialysis is appropriate for elderly patients. Contrib Nephrol. 2006;150:240-6.
- Dimkovic N, Oreopoulos DG. Chronic peritoneal dialysis in the elderly: a review. Perit Dial Int. 2000 May-Jun;20(3):276-83.
- Dimkovic NB, Prakash S, Roscoe J, Brissenden J, Tam P, Bargman J, Vas SI, Oreopoulos DG. Chronic peritoneal dialysis in octogenarians. Nephrol Dial Transplant. 2001 Oct;16(10):2034-40.
- Sunder S, Taskapan H, Jojoa J, Krishnan M, Khandelwal M, Izatt S, Chu M, Subramanian P, Chinthalapalli H, Lobbedez T, Jassal SV, Bargman JM, Oreopoulos DG. Chronic peritoneal dialysis in the tenth decade of life. Int Urol Nephrol. 2004;36(4):605-9.
- Clinical Practice Guidelines and Clinical Practice Recommendations for Peritoneal Dialysis Adequacy, Update 2006. Am J Kidn.ey Dis July 2006 supplement
- Davies SJ, Brown EA, Frandsen NE, Rodrigues AS, Rodriguez-Carmona A, Vychytil A, Macnamara E, Ekstrand A, Tranaeus A, Filho JC; EAPOS Group. Longitudinal membrane function in functionally anuric patients treated with APD: data from EAPOS on the effects of glucose and icodextrin prescription. Kidney Int. 2005 Apr;67(4):1609-15.
- Duman S, Asci G, Toz H, Ozkahya M, Ertilav M, Sezis M, Ok E. Patients with failed renal transplant may be suitable for peritoneal dialysis. Int Urol Nephrol. 2004;36(2):249-52.
- Davies SJ. Peritoneal dialysis in the patient with a failing renal allograft. Perit Dial Int. 2001;21 Suppl 3:S280-4.
- Badve SV, Hawley CM, McDonald SP, Mudge DW, Rosman JB, Brown FG, Johnson DW; ANZDATA Registry PD Working Committee. Effect of previously failed kidney transplantation on peritoneal dialysis outcomes in the Australian and New Zealand patient populations. Nephrol Dial Transplant. 2006 Mar;21(3):776-83. Epub 2005 Nov 9.
- de Jonge H, Bammens B, Lemahieu W, Maes BD, Vanrenterghem Y. Comparison of peritoneal dialysis and haemodialysis after renal transplant failure. Nephrol Dial Transplant. 2006 Jun;21(6):1669-74. Epub 2006 Feb 9.
- Twardowski ZJ. Presternal peritoneal catheter. Adv Ren Replace Ther. 2002 Apr;9(2):125-32.
- McDonald SP, Collins JF, Rumpsfeld M, Johnson DW. Obesity is a risk factor for peritonitis in the Australian and New Zealand peritoneal dialysis patient populations. Perit Dial Int. 2004 Jul-Aug;24(4):340-6.
- Aslam N, Bernardini J, Fried L, Piraino B. Large body mass index does not predict short-term survival in peritoneal dialysis patients. Perit Dial Int. 2002 Mar-Apr;22(2):191-6. Comment in: Perit Dial Int. 2002 Sep-Oct;22(5):634-5; author reply 635-6.
- McDonald SP, Collins JF, Johnson DW. Obesity is associated with worse peritoneal dialysis outcomes in the Australia and New Zealand patient populations. J Am Soc Nephrol. 2003 Nov;14(11):2894-901.
- Vonesh EF, Snyder JJ, Foley RN, Collins AJ. Mortality studies comparing peritoneal dialysis and hemodialysis: what do they tell us? Kidney Int Suppl. 2006 Nov;(103):S3-11.
- Harel Z, Wald R, Bell C, Bargman JM. Outcome of patients who develop early-onset peritonitis. Adv Perit Dial. 2006;22:46-9.
- Cox SD, Walsh SB, Yaqoob MM, Fan SL. Predictors of survival and technique success after reinsertion of peritoneal dialysis catheter following severe peritonitis. Perit Dial Int. 2007 Jan-Feb;27(1):67-73.

