Physician Bedside Manners and Ableism

This blog post is inspired by my lifelong experience as a disability rights advocate. I was born disabled and have been in a wheelchair since I was ten. So, I have always known about the discrimination that goes on towards those us with disabilities and chronic illness.
Just as the oppression and the discriminatory practices against people of color or another gender are called racism and sexism, discrimination against people with disabilities and chronic illnesses is called ableism. And it is indeed something we see all the time.
Often ableism is so subtle and implicit that it is not even seen as an oppressive practice. I see it in particular when I go to the hospital, where doctors excel in doing so. Many of them feel that with their long education and specialization, they are experts on my disease, its treatment—and on how I should live my life. They assume a role where they are the only ones who are credible enough to have knowledge of my disease and to make a decision as to what is going to happen to me going forward. In assuming expertise many ignore the fact that I have spent years—if not a lifetime—with my condition. I have spent more than the 10-15 years they used in med school with my kidney disease. Not only that, but I had the privilege of concentrating on one specific disease in one specific patient, while they had to learn about everything from ingrown toenails to advanced cancer and heart disease. Not that they wasted their time—they still know the overall picture of what goes on in the body. But I know what my disease does to my body in a way they will never understand.
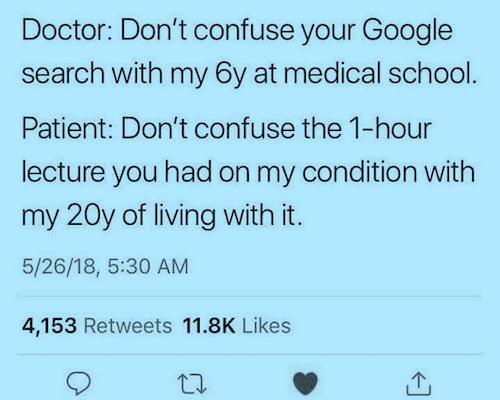
So, the attitude of I-know-so-much-better-than-you-what-is-best-for-you-and-you-just-sit-and-be-quiet-while-I-talk is a blatant example of ableism. It is subtle, and many will never recognize it. But it makes us patients docile (a synonym for compliant, btw) and that is how many want us to act. Docile, compliant patients are easier to handle, however, they also are treated far more poorly, because contrary to what they might think of themselves that type of doctor is not God.

So, this blog post is a call to arms. We need to be much better at knowing what goes on with our bodies. The first thing as a dialysis patient is to know your lab results:
What does it mean that your PTH is high?
What consequences does it have?
Now?
And, 10-20 years from now?
I mean, don't you want to live that long? You need to be able to recognize the most blatant things that can go wrong. Remember that in some countries (including the United States), a doctor can specialize in nephrology without knowing more than the absolute most rudimentary things about dialysis. It is simply not as interesting as things connected to transplantation, even if only a fraction of those of us with kidney failure end up getting transplanted.
I know not everyone is a nerd like me. Many are not interested in knowing these things. Others are not able to do so. But what we can all do is to assert ourselves and demand to be treated as equals. That means, if the doctor demands that you act in a certain manner or they push a certain treatment regime or medicine on you the first questions out of your mouth should be why? What is the purpose of this? Why didn't you ask me if I was interested in doing as you just told me? I might have other priorities than the ones you are trying to cram down over my head…
In my world, the first thing a doctor should always ask his/her patient are questions like:
What is your goal of coming today?
Or, what do you want out of life?
If they don't ask (which is the case 99% of the time) volunteer that information. And if/when they interrupt you, simply ask: "How do you expect you can treat me for anything if you don't give me the time to let you know why I am here?"
Knowing what a patient wants and expects is the basis for all respectful doctor-patient relationships. And if that is not possible, run for the door and find another doctor. Because if you settle, suboptimal and potentially lethal treatment is lurking on the horizon.


Comments