Combatting Implicit Bias in Home Dialysis

Each month, I scan through the abstracts of every newly published peer-reviewed journal article about dialysis to put together the Home Dialysis Central e-newsletter. This month, I was dismayed to find an article by Hofacker et al reporting data on CPR performance in dialysis from the Cardiac Arrest Registry to Enhance Survival (CARES) surveillance group (NOTE that CARES excludes patients who have a DNR order in place). Unfortunately, the news was dire: “Black and Asian patients are significantly less likely than white patients to receive CPR from dialysis staff.” In their analysis of 1,568 cardiac arrests from 809 dialysis clinics, 91% of white patients, 85% of black patients, and 77% of Asian patients received CPR from staff. Appalling!
We have certainly had other indications of bias in nephrology, as with everywhere else. It’s long been the case that people of color have been less likely to do peritoneal dialysis (PD) or home hemodialysis (HD) than whites, for example. Mehrotra et al reported in 2016 that “Every racial/minority group was significantly less likely to be treated with home dialysis than whites.” Dr. Keisha Gibson spoke at the virtual ASN meeting this month, noting that systemic racism, implicit bias, and structural oppression must be addressed if we are to achieve health equity in the U.S. Even the eGFR equation is now suspect, as it underestimates the risk of kidney disease progression among Black and Hispanic people—which underscores the fact that even numbers may not be as “objective” as we may think..
The Institute of Medicine (IOM) has identified health disparities for a variety of groups, including:

- African Americans
- Appalachian poor
- Certain religious minorities
- Immigrants and refugees
- Latinos/Hispanics
- Members of the LGBTQIA community
- Native Americans
- Overweight people
- People with disabilities
- Prisoners
- Seniors
- Women
Even children are not exempt from healthcare bias. One devastating study (from the pre-opiate-awareness era) found that pediatricians with higher degrees of measured implicit bias were more likely to recommend post-surgical narcotics to white children than to black ones.

What is Implicit Bias?
Implicit bias favors our own in-group—unconsciously, and perhaps even counter to our own values. Who is our “in-group”? We each have multiple in-groups, or “people like us.” Some groups are based on things we can see at a glance—like age, race, gender, weight. Others are based on things we learn about people once we get to know them, like politics, sports teams, church membership, favorite crafts, or preferred pets.




Our human tendency (see figure 2.1 below) is to treat people outside of our own in-group(s) as “other,” and therein lie our interpersonal and intergroup challenges. In the early days of humans, “others” may well have been rivals for food or territory, but today many of us live close together in enormous population clusters. Some of our most urgent existential threats are only likely to be successfully addressed by collaboration, not competition. We need to learn new ways to work together, perhaps even to survive as a species. And, in healthcare particularly, we need to rid ourselves of biases that could harm patients.
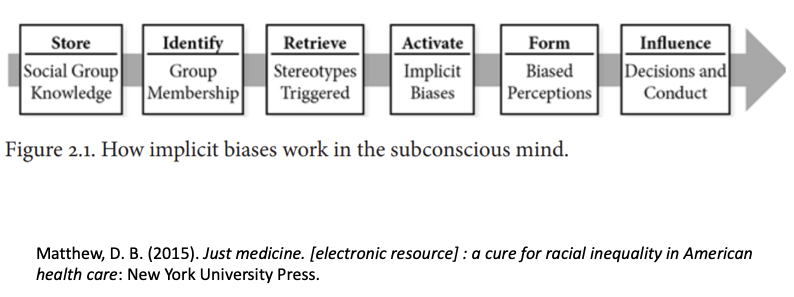
NOTE: You can watch Dr. Dana Bowen Matthew, author of Just Medicine, in a Youtube lecture.

As a nephrology community, we may not be able to do much about the systemic racism suggested by the IOM—except to try our best as individuals and through policies and procedures to be antiracists. (While how to do that is outside of the scope of this post, Ibram X Kendi’s book can help.) And, we may not be able to overcome structural oppression as individuals. But, we can learn about and manage our implicit biases. And, we need to do this work.
How to Address Our Own Implicit Biases Around Home Dialysis
Assessing our implicit bias is not, unfortunately, straightforward. An Implicit Association Test touted by Harvard is all over the Internet. But, the IAT requires a computer and keyboard and is challenging to take, with fiddly requirements to hit certain keys while looking at faces and words, and instructions that change with each section. The IAT is a good starting place for self-reflection, but it is not reliable for individuals, only for populations.

Fortunately, we can improve our sensitivity to other perspectives through acts like reading books written about other cultures. One of my favorites is a story of a 2-year old Hmong child with epilepsy, The Spirit Catches You and You Fall Down, by Anne Fadiman.
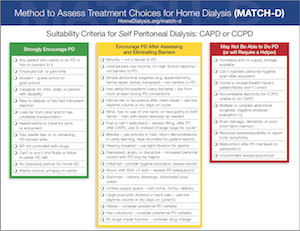

And, we can act to challenge our implicit bias even without a full diagnosis of where, exactly, our own fall. One of the best ways to do this for home dialysis is to obtain input from a variety of people. When Beth Witten and I developed the MATCH-D in 2007, our process was to reach out to dozens of PD and home HD experts from around the world to ensure a range of points of view. Following three rounds of comments and edits, we had a free tool that has been widely adopted across the nephrology community to help reduce bias in patient selection for home therapies.
Similarly, the My Life, My Dialysis Choice treatment matching tool that Beth, Dr. John Agar, and I developed helps us all to route around our own biases about who might be interested in which treatment option(s) by incorporating evidence-based information and having each patient choose several top values and rate each option as it suits his or her life. This free tool, into which we incorporated comments from more than 200 reviewers, is listed in the Ottawa Hospital Research Institute (OHRI) compendium of patient decision aids, and meets all of the criteria of the International Patient Decision Aid Standards (IPDAS).
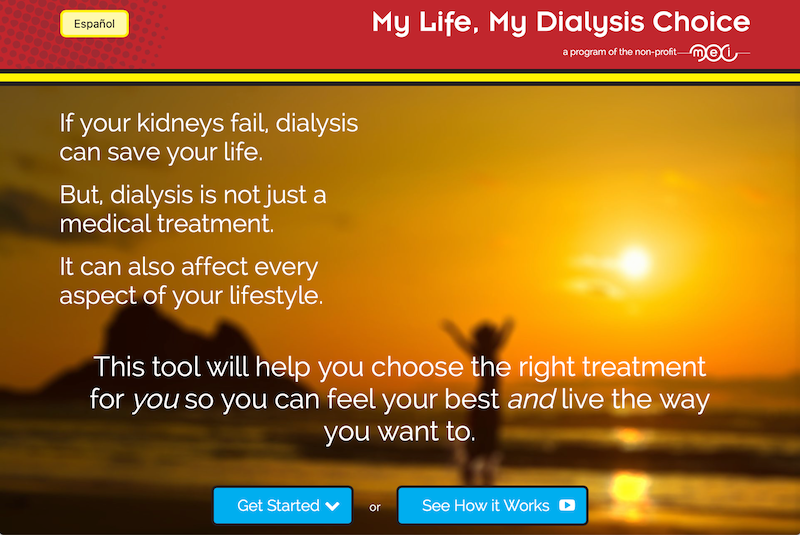
Together, these FREE tools make a powerful one-two punch to help us combat our own implicit biases toward patients and their biases about which options might be acceptable to them.
Conclusion
We count on healthcare providers to use their internalized practice wisdom to make decisions. But, we are all subject to biases. And, while the sort of algorithmic thinking used in healthcare is designed to save time, money and resources—it does not always save lives. The key is to be aware of and manage our biases when we participate in the care of patients. It is important that we recognize the biases we have and work hard to make sure our biases do not lead us to limit our patients’ choices and opportunities to live the lives they want to live—which may or may not include learning about and considering PD, home HD, or transplantation.


Comments
Dori
Jan 10, 2021 5:28 PM
Yvonne Coleman
Jan 10, 2021 3:13 AM