Training for Home Haemodialysis in the U.K.

So much has happened recently in my dialysis world that I have a feeling this first blog of mine is going to be super-long…so apologies in advance! I hope my experiences are useful to other patients on their home dialysis journey.

After 2 years of dialysis in a satellite unit in Darlington, in the north east of England, about 3 weeks ago the wheels really started getting into motion. Throughout my time in the satellite unit, I have been encouraged by the staff to become completely independent in my treatment. I was lining and priming the machine within a month, connecting my neckline catheter soon after, and when my fistula was ready, in around January 2021, was taught how to needle myself and create a buttonhole. Consequently, I have become completely independent and have required no nursing intervention for quite some months now. This has really helped the transition to home haemo go smoothly and as rapidly as possible.
I began to enquire about home haemodialysis when I separated from my husband and moved house. Being tied to the unit three times a week was becoming increasingly difficult to balance with childcare, and I was itching to get back to work and start socialising more flexibly. At first, my renal team at James Cook University Hospital was reluctant. They were worried about the risks involved in me dialysing alone at home while my children (7 and 4) were in the house. I was determined, however, and began to think of contingency plans and options that would make home dialysis as safe as possible for myself and my children. I contacted an advocate at Kidney Care UK and chatted to other solo patients on Facebook groups. After speaking to my consultant again and agreeing to only dialyse when the children weren’t at home alone with me, it was agreed that home haemodialysis would go ahead.

The first step was for the home haemodialysis nurse from James Cook to visit me at home. She chatted about the process, provided me with photographs, testimonials and other information, and checked the room where the machine would be installed. I believe that in the past in the UK it has been the case that patients must have a separate room for their treatment, but it is now possible to have the machine installed in a bedroom. I am hoping to be able to do nocturnal dialysis once settled, so I asked for the equipment to be installed next to my bed. The nurse simply checked there would be enough room; I was anxious that she would be inspecting my house, so I probably spent too much time frantically cleaning and decluttering before her visit!
Following this, I had a visit from a surveyor from the company that would be installing the equipment. He checked that the electrics, water and drainage were suitable. It was touch and go for a while, as he was unable to see a way to install the draining from the machine. He explained that the waste from dialysis is more viscous than water so requires a good “fall” angle on the pipe; unfortunately, my machine is on the opposite side of the house to the mains waste pipe, so an imaginative solution had to be found. Luckily, the surveyor thought carefully and was clearly determined to make it work for me. For this I am very grateful!
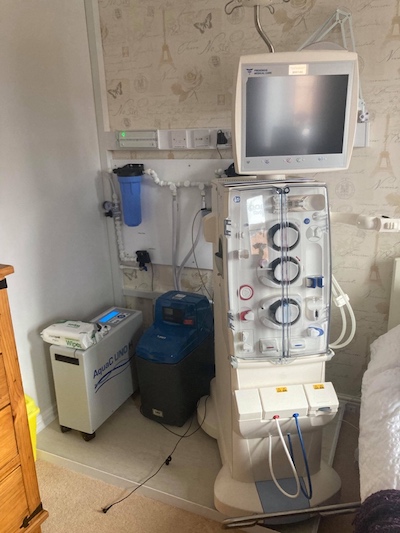
After this was solved, the home haemo nurse arranged for me to dialyse at James Cook while training on the dialysis machine. Unfortunately, the machine that is used at home is different to the one I have been working with at the satellite unit for 2 years, so I had to go back to the beginning and start again with lining and priming and understanding how the machine works.
The plumbing for the equipment was installed in just over half a day by two men. They did not require any help or preparation from me; they moved the furniture, provided all equipment and plumbed everything in. Before they left, they explained and demonstrated how some of the equipment works. As you can see from the photograph, it’s very “hospital-like.” I had seen photographs and I thought I knew what to expect, but when you see it in your own house it is a little disconcerting, and to honest, I didn’t like sleeping next to it very much!

Soon after the plumbing was installed, the dialysis machine was delivered, then the “RO” (reverse osmosis machine) was delivered by the technicians from the hospital, who came and spent a day setting everything up. Another delivery (of acid and bi-bags) came from Fresenius, then another delivery (of lines, needles, dialysate, tape, gloves, plasters, salt, medication etc., etc., etc.!) came from the hospital. There was also a pack of paperwork tocomplete during treatment and an order form for my next delivery of supplies. The photographs show shelving in my garage, where I’m keeping the majority of supplies, and shelving in a cupboard upstairs where I’m keeping around a month’s worth of supplies. There is quite a lot of equipment and medical supplies involved with home haemo so storage space is a must, but I am determined not let my bedroom get completely “hospital-ised,” so I decided to keep most things hidden away. I will gather up everything I need for each treatment.

One of the surprising things about home haemo, that dialysing in hospital does not prepare you for, is how noisy the equipment is! The RO machine must carry out self-cleans and rinses periodically, and must also run throughout treatment. Clearly this process is done on a larger scale “behind the scenes” at the unit, so I wasn’t ready for a 6am whooshing, humming, and dripping alarm clock! The machine can be set to rinse and clean at times convenient to you, but it must be done every 8 hours. I haven’t yet done a treatment at home, but think that if I can used to the patients on the unit who snore throughout their 4-hour treatment, I can get used to the sound of the machine running its cleaning programme!
I have now been training at the hospital for six sessions, and am hoping to do just two more before coming home with the supervision of a nurse. I feel as though I am making good progress, but do find it frustrating having to learn a different machine from the beginning again! Unfortunately, I had a setback last week which has extended my time doing in-hospital training. Not long into Monday’s treatment, the machine began alarming due to incorrect venous and arterial pressure. I tried lowering the blood flow and repositioning my arm but the blood in the lines when extremely dark in colour and the alarms didn’t stop. After stopping treatment, a nurse discovered that my fistula wasn’t working at all; we couldn’t hear or feel the “thrill.” The nurse sprang into action, booking an urgent ultrasound scan, which showed that there was a 4 centimetre blood clot in the vein. I was then taken straight into urgent surgery to repair the fistula. A blood test showed that my potassium level was dangerously high, so it was of utmost importance that the fistula was repaired. Luckily, and with huge thanks to the surgeon, after 2 hours he managed to complete the surgery. The surgeon said he had “70% confidence” that it would work, so it was a tense time overnight until, thankfully, I could hear and feel the “thrill” in the morning. I had medication to take to lower my potassium, and was afraid to eat or drink anything, in case I couldn’t dialyse the next day.
I feel that this happened at the “right” time: I was at the main hospital, where a repair could be done quickly, and my children are currently away on holiday with their dad. Dialysis—and the issues caused by it—can really get in the way of life. I have always lived by the idea that I dialyse to live, as opposed to live to dialyse, but appreciate just how difficult that can be in practice. I am determined to get back to my career as a teacher, and don’t want to have to plan my life around having to be in the hospital 3 mornings a week and recover from treatment 3 afternoons a week. I am very much looking forward to having the ability to plan dialysis around my life by dialysing at home in the coming weeks. I will keep you updated!


Comments
Glenda V. Roberts
Sep 03, 2021 4:53 PM
Great pictures that reinforces the hospitalization of the home. I’d never thought about the noise that the machine would make while it was being cleaned.
With your commitment, given the other life challenges, I am confident that you will get home. Email me at glendar@kri.washington.edu so that I can follow your blog post.
Amy Staples
Sep 03, 2021 2:18 AM