Buttonhole Cannulation Revisited: A Procedure for Safe Scab Removal to Prevent Infection


As with most trends in our society, things that were once given top billing fall out of the public limelight—and then resurface with a new look. The buttonhole, or same site cannulation technique, was once lauded as the humane cannulation method for hemodialysis patients with AV fistulas for minimizing patients' fear of needles, decreasing cannulation pain, and potentially increasing fistula lifespan.1 Unfortunately, since its inception by Dr. Twardowski in 1977,2,3 this technique received a bad reputation due to the increased number of infections associated with the procedure.
A closer look at the reason behind these infections suggested that inadequate removal of the scab that forms over the needle stick site post-dialysis may have been responsible.4 The routine method of removing the scab with tweezers, pickers, or needles, resulted in residual scab fragments and tears of the skin at the exit site. The scab fragments were then pushed into the needle track during cannulation, introducing bacteria into the tunnel and bloodstream.5 Tearing of the skin around the mouth of the exit site caused breakdowns of the skin's protective barrier, an increase in the potential for bacterial growth at the site, and a resultant production of scar tissue leading to “mound” type of skin formation at the needle site and thicker, harder to remove scabs.

Stuart Mott, a longtime advocate of the buttonhole method, introduced a more stringent process for scab removal that decreased the risk of infection when using buttonhole cannulation. Mott promoted removing the scab using a reusable cosmetic scrub pad and tap water. He was able to document buttonhole cannulation sites that were well-healed and exhibited minimal tears in the skin around the scab removal sites.6
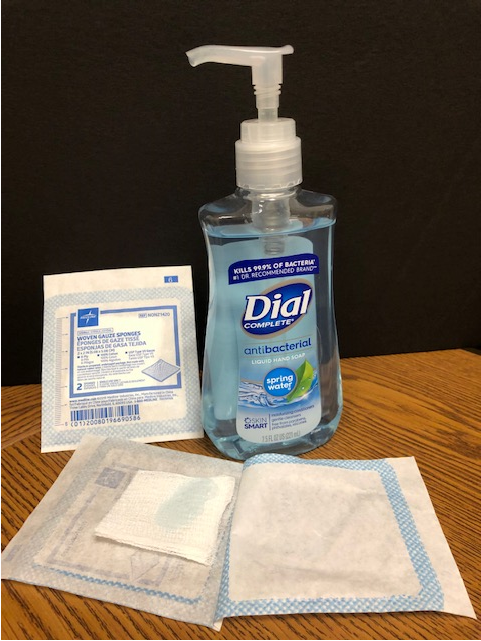
After a closer evaluation of Mott's scab removal method, staff at the University of Vermont Medical Center (UVMMC) Home Dialysis Program made some minor changes to the procedure, using a sterile 2x2 in place of the cosmetic scrub sponge, and adding a longer soaking period with antibacterial soap. This change to the process resulted in an immediate decrease in needle site infections in our patient population. We have continued to use this method of scab removal with excellent results. These buttonhole sites heal quickly and remain free of the scar tissue formation.
The procedure is as follows:
-
Soak the cannulation site with a sterile 2x2 and antibacterial “pump soap” for 10 minutes.
-
Remove and discard the wet 2x2.
-
Wipe away the scab with a fresh sterile 2x2, using gentle friction. Be sure to remove the scab in its entirety. If scab fragments remain, repeat the soak and remove steps.
-
NOTE: AVOID USE OF “PICKERS” OF ANY KIND.
Since initiation of this process in the UVMMC home clinic in 2014, there have been only 2 access infections—both of which were a result of patients' admitted deviance from the program's procedure.7 Mott, has since embraced the changes and has also been able to reference buttonhole cannulations without infections in multiple facility sites.
While our results derive from observational cohort data, rather than a structured randomized study; the outcomes demonstrate a real potential for the buttonhole cannulation method to be to be an effective technique that should be revisited by facilities training home dialysis patients, in-center assisted care patients, or in-center facilities that can support designated cannulators.
I encourage all providers who are currently advocating/utilizing the buttonhole method for their patients, and those who have avoided it due to the infection risk, to review the references for this post and strongly reconsider implementing the scab removal process as outlined. It is my hope that the buttonhole method will once again be seen as a viable, safe method of cannulation and that patients will be offered and educated on this method.
References
Allon M. Is it time to abandon buttonhole cannulation of arteriovenous fistulas? Kidney Med. 2019 Sep 12;1(5):235-237 ↩︎
Twardowski Z et al. 6-year experience with creation and use of internal arteriovenous fistulae in patients treated with repeated hemodialysis. [Polish]. Pol Arch Med Wewn. 1977 Mar;57(3):205-213 ↩︎
Twardowski Z. Update on cannulation techniques. J Vasc Access. 2015;16 Suppl (9):S54-S60 ↩︎
Ball LK. The buttonhole technique: strategies to reduce infections. Nephrol Nurs J. 2010 Sep-Oct;37(5):473-7, quiz 478 ↩︎
Nesrallah GE. Pro: buttonhole cannulation of arteriovenous fistulae. Nephrol Dial Transplant. 2016 Apr;31(4):520-3 ↩︎
Mott S, Moore H. Kinder, gentler methods for scab removal in buttonhole access. Nephrol Nurs J. 2010;38(5); 439-43 ↩︎
Bushey, M. Buttonhole cannulation of arteriovenous fistulas: a dialysis nurse's perspective. Kidney360. 2020 Apr;1(4):279-280 ↩︎


Comments
kazuhiko shibata
Apr 13, 2022 8:51 AM
Dori Schatell
Jul 31, 2022 5:22 PM