Why Shared Care was Important to Me

This is my renal story and shared care is an important part of it—in fact, it might be the central part, the keystone that supports the arc of my story.
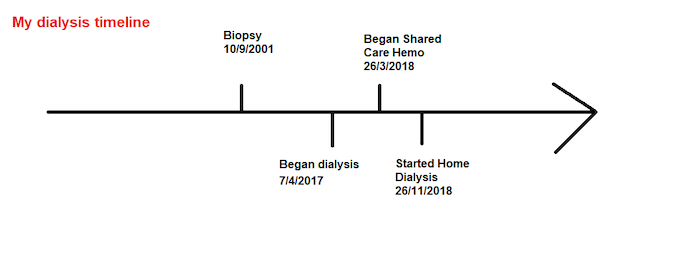
In 2001 I had a renal biopsy which confirmed the working theory that I had a chronic kidney disease (CKD). It is an immune system issue which affects my kidneys called IgA Nephropathy. There is no cure, and eventually it would stop my kidneys from working.
My kidney function slowly declined over the next 17 years, until in 2017 they weren’t working well enough and I had to begin dialysis. I started on peritoneal dialysis (PD), which I could do at home, but it was soon clear to my nephrologist and nurses that it wasn’t working well enough for me and I needed to come to hospital for haemodialysis (HD). I resisted and spent an extra 6 months feeling worse than I needed to!

But into hospital I came, from 26 March 2018. HD is a regular treatment typically 3 days a week for 4 hours. I’d explained to the nursing team that I wanted to retain as much independence as I could, and I was placed on the Shared Care bay in the Renal Unit—which meant I’d be taught how to do some of my care myself. How much was up to me, and there was no time limit placed on how long I needed to take to learn; meaning I could take things at the pace that I was comfortable with.

We started on day 1 session 1. Ben, my nurse, explained to me how dialysis works—what would be happening while I was on treatment. He showed me how to wash my hands properly and to clean my fistula. Then, he asked me to put the “lines” onto the machine—the tubing that would be used shortly for the treatment. He explained what went where on the dialysis machine, and how that all related to what he’d explained.
I’ve been lining my own machine ever since. For a few weeks I needed guidance and help to remember what went where, not touch the tubing ends, keep the tubes uncrossed, etc., but, gradually the process began to become routine and comfortable.
Once I was comfortable with lining the machine, I was shown how to take my own blood pressure and to record my weight, and—more importantly—why this information is so important in dialysis!
For me understanding WHY makes learning HOW so much easier! “This is how we weigh you and this is why we do it, and then this is what we do with that information.”
In the months that followed I learned more and more about dialysis, about fluid movement inside the body, about the impact of sticking to/not sticking to the food and fluid restrictions, and about the effects of dialysis on MY body. I became fully engaged in MY treatment. This made me a better patient and more able to properly discuss my renal failure and dialysis with the doctors and nurses. My new nurse, Kate, was fantastic at helping me learn and then apply that learning to my treatment.
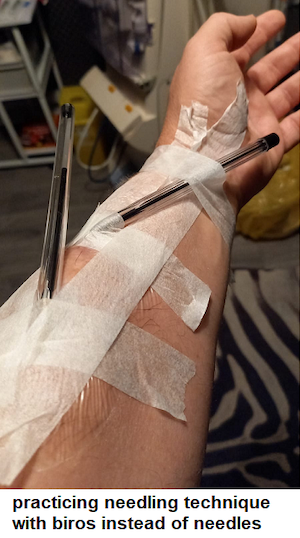
For me, though, the hardest part was learning to deal with the needles! It took me months to be ready to try to put them in myself. Eventually, I was ready to try, after a couple of weeks training on tubing set up just like my fistula so I could practice the exact motion I’d need to use when I did it for real. I did it! Then I was in floods of tears—from a mix of a release of stress, the realisation that I’d have to do this again and again, and pride that I’d overcome a huge fear.
Over the next hour, there was a steady stream of nurses coming to say, “Well done!” as the news of this major triumph for me tom-tom-ed its way around the ward. That moment of success was shared and celebrated by everyone that had helped me and cared for me in the previous months – perfectly illustrating for me how Shared Care is a collaboration, not an attempt to remove nurses from treatment.
With the major hurdle of needles out of the way, my thoughts then turned to getting full autonomy and a desire to move to home dialysis. This was not an automatic step. I’ve heard patients say they didn’t
want to start shared care because they were worried they’d then be forced to go home, but that’s not the case at all. Many patients remain in their unit in full control of their treatment, remaining on shared care. Others, like me, used it as a stepping stone to then choose home dialysis. The key thing for me is that it is a choice that is yours to make—but you can only make it by taking the first step.
I’d recommend that every dialysis patient talk to their team about doing some shared care. It was the way I began to thrive on dialysis.


Comments
Susan Emeny
Jul 28, 2023 12:34 PM
This is just my opinion. :)
Theodôr Vogels
Jul 28, 2023 6:01 AM
But shared care starts with the support and chances provided by your team and whatever the outcome I encourage each patient to carefully explore what you need and be satisfied even if you do not achieve full self care. Just get what you need at the level you are comfortable with in the end. Although working abroad in the Netherlands: Attune the treatment to the patient and those closest...that has always been my motto as a nephrology social worker! 😃